|
|
Quiz Me! |
Immune Response: B- and T-cell biology |
|
|
|
Lecture Index | ||
|
|
Course Resources page |
Last revised: Friday, January 7, 2000
Ch. 31 in Prescott et al, Microbiology, 4th Ed.Note: These notes are provided as a guide to topics the instructor hopes to cover during lecture. Actual coverage will always differ somewhat from what is printed here. These notes are not a substitute for the actual lecture!Copyright 2000. Thomas M. Terry
T-cells and T-cell receptors
- T cells mature in the thymus gland, and differentiate further into several varieties which can be distinguished based on whether they carry surface proteins of type CD4 or CD8.
- CD4 = T-helper cells, T-delayed-type hypersensitivity
- CD8 = T- cytotoxic cells, T- suppressor cells
- T cells don't produce antibodies. Each T cell, however, is different from its fellow T cells in having the capacity to recognize only one very specific antigen by specific T cell receptors (TCRs).
- TCRs have certain similarities to antibodies--constant and variable regions, specific binding sites, millions of different specific varieties.
- An antibody can recognize an antigen (e.g. the surface protein of a bacterium) floating around in blood, in a pool of cell debris, in a test tube, etc. But a TCR can't do this--it can only recognize an antigen if the antigen is bound to a certain type of protein, MHC.
MHC proteins
- MHC protein = "major histocompatibility complex", binds to fragments of an antigen, carries to cell surface, "presents" antigen.
- The only way for an antigen to get to this position is by being partially degraded inside the cell, then carried to the surface and bound to an MHC protein.
- Over 100 diff. alleles of MHC in humans. Each person has only 2 (1 if homozygous). Tissue rejection occurs if MHC proteins on transplanted tissue are different from self (which usually is the case).
- Two major classes of MHC proteins:
- Class I MHC proteins (found on the surface of all nucleated cells) present antigens, identify most body cells as "self", detected by T cytotoxic or TC cells.
- Class II MHC proteins (found only on B lymphocytes, macrophages, and other cells that present antigens to T cells) don't stimulate antibody production, but are needed for T-cell communication with B-cells and macrophages.
- View MCH molecules (requires Chime plug-in)
- The importance of MHC proteins is that they allow T cells to distinguish self from non-self. In every (nucleated) cell in your body, antigens are constantly being chewed up and "presented" for inspection by passing T cells. Until this happens, other aspects of the immune response (such as antibody formation) cannot happen
- Note that the when class II MHC proteins present antigens, they are detected by a different group of T cells (called T-helper or TH cells) than class I MHC proteins (which are detected by T cytotoxic or TC cells).
Cell-mediated immunity
- T cells can participate in a variety of functions (see Fig. 20.18). Note that circulating lymphocytes are mostly T cells, of different types (B cells are typically found in lymph nodes).
- Some examples of T-cell functions:
- Cytotoxic T cells (TC cells) can recognize "foreign" antigens (e.g. from a cancer, or a virus infection) carried by MCH class I molecules. Once the T-lymphocyte recognizes an infected cell, it produces a set of new proteins that it places on the surface of the other cell. Those proteins then bind to receptors on the infected cell called "death domain receptors" (including the Fas ligand and Trail receptors). This binding triggers a cascade of events in the infected cell that leads to cell suicide, called apoptosis (pronounced A-pahtosis).
- T-helper cells (TH cells): required for B-cell activation. View diagram showing activation of TH cells.
- T-suppressor cells (TS cells): prevent induction of TH and B cells.
- Delayed-type hypersensitivity cells (TDTH cells); mediate delayed reactions. Won't discuss in this course.
- Another example of cellular immunity is the stimulation of phagocytic activity in macrophages by cytokines ( called lymphokines when released from T lymphocytes), specific signals released by one cell population to control activities of other cell populations.
- Cytokines include a variety of proteins:<
- Interleukins = proteins that signal between white cells in immune system.
- Migration inhibitory factor (MIF). Inhibits migration of macrophages away from site of infection.
- Colony-stimulating factors (CSFs). Regulate production of phagocytic cells.
- Interferons. Help in developing antiviral properties. Interferons also modulate immune response, cause increases or decreases in B- and T-cell functions.
Clonal selection
- Antibody synthesis occurs by clonal selection, and involves a number of steps:
- there must be a wide variety of T and B cells containing different specificities for a wide variety of antigens;
- when a particular antigen is present, it becomes exposed on the surface of some cells in the body (e.g., after ingestion and presentation by a B cell or macrophage) in a complex with class II MHC protein;
- a TH cell with corresponding specificity for this particular antigen on its TCR binds to the B cell, and is triggered to release interleukins that stimulate further division of the relevant B cell to form many copies of itself (a clone);
- Note: some antigens can stimulate B-cell activation without needing T-cell (= T-independent antigens). Ex: LPS.
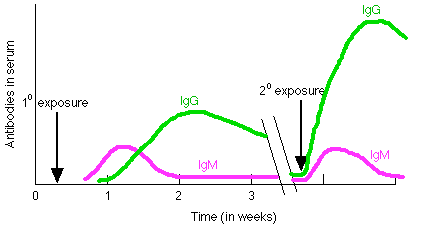
Primary and Secondary Immune responses
- Primary response: requires ~ week after exposure before Ab level in blood rises. IgM appears first, followed by IgG.
- Secondary response: activates memory cells, Ab response detectable within a day, much higher Ab levels, higher IgG response.
Immunization and Vaccines
- Immunization can be active or passive
- To get active immunity, need challenge with antigen without causing significant disease. Several considerations:
- toxoids = inactivated toxins
- live vs. killed vaccines
- engineered vaccines
Superantigens
- Superantigens are produced by certain strains of staphylococci and streptococci; a common example is toxic shock syndrome, brought about by a staph toxin.
- Superantigens bind to beta-chain of T cell receptor, at a site outside normal Ag-binding site. Can stimulate up to 10% of all normal T cells in population --- results in simultaneous and enormous amount of cell-mediated response = systemic inflammatory response.
Take a Self-Quiz on this material
Return to Lecture Index
Return to MCB 229 Course Resources page